Pediatric suicides have not increased in the US during the pandemic
Data from the CDC extending to September 2022 shows no evidence of a "tsunami" of suicide deaths in children under 18 years of age.
We now have 31 months of US pandemic data on suicides for kids under 18 years old, using the CDC Wonder data portal. I have been able to create estimates to account for data lag, so this data is highly reliable as the final numbers.
The Data
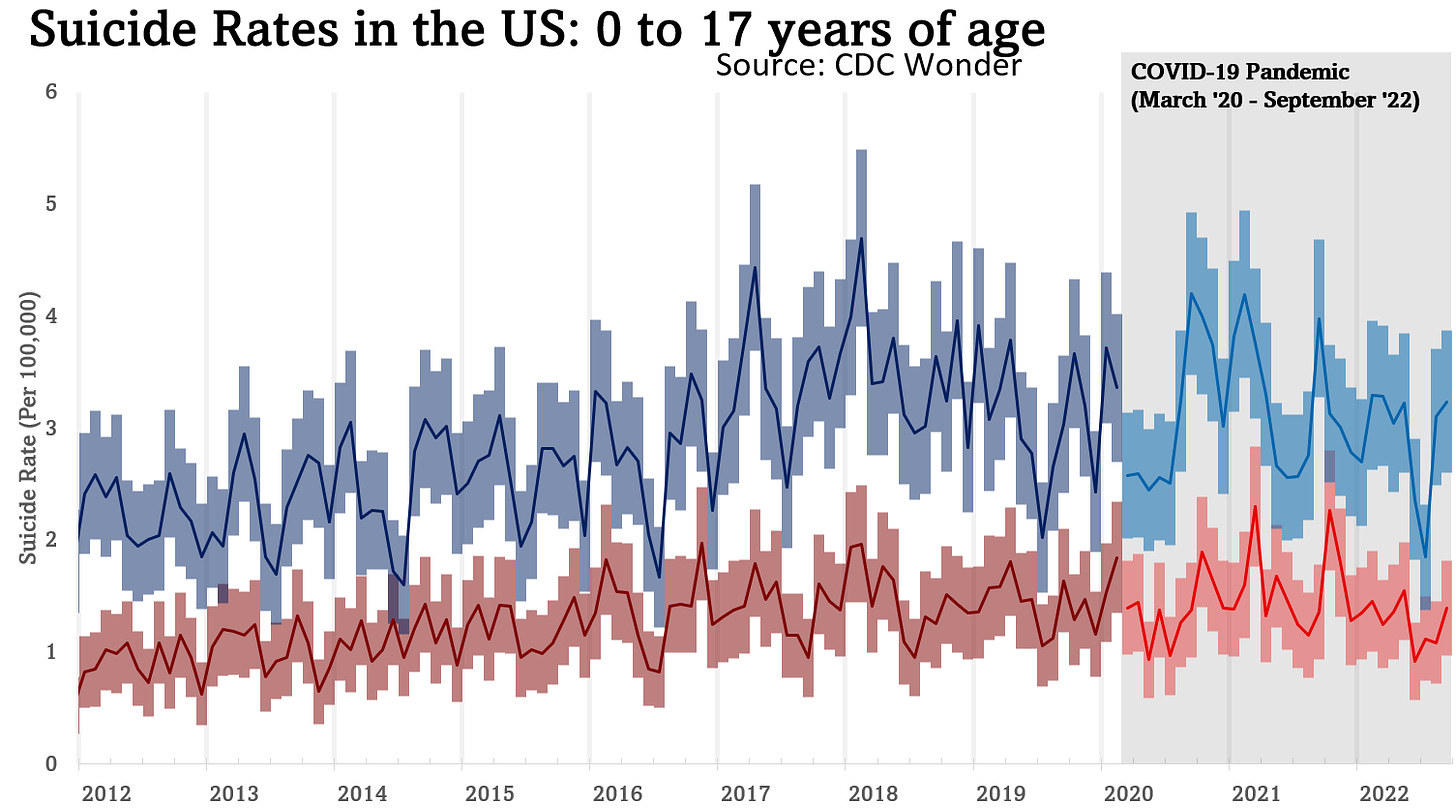
Visually, there has been no increase in suicides up to September 2022. Despite concerns, there has been no tsunami or delayed effect of the pandemic on suicides among children.
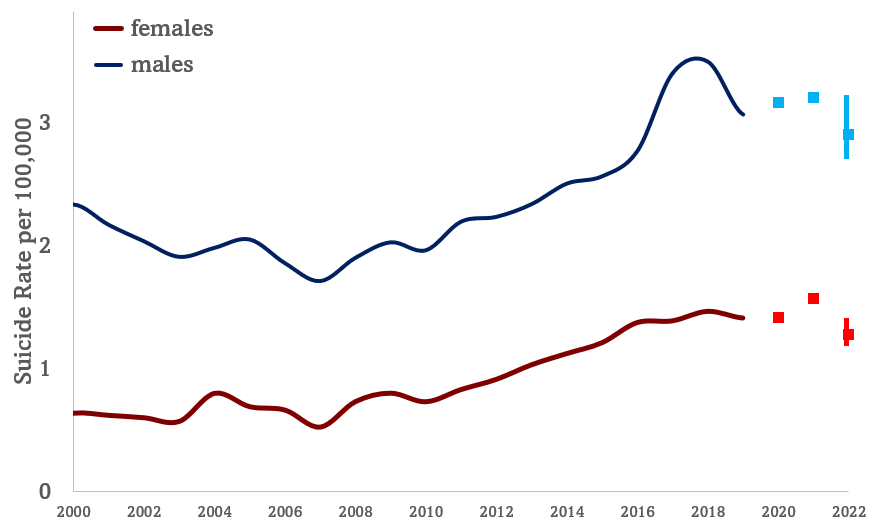
To further support this finding, we can examine the data on a year-by-year basis. This visual check compares yearly suicide rates by sex. The data is broken down for both male and female suicide rates from 2020 to 2022, and it is evident that these rates are within the expected trends. There have been no unexpected increases in suicide rates for either males or females during this time period.
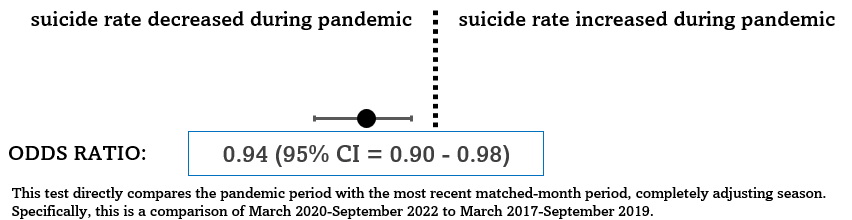
Continuing our analysis, we can also perform a statistical check using month-matched odds ratios. By directly comparing the 31 months starting in March 2017 to the 31 months starting in March 2020, we can better understand the impact of the pandemic on child suicides.
Interestingly, there is some evidence of a net decrease in child suicides by 6%. An increase in suicides during this period is statistically unlikely, further dispelling the notion that the pandemic has led to a significant rise in suicide rates among children.
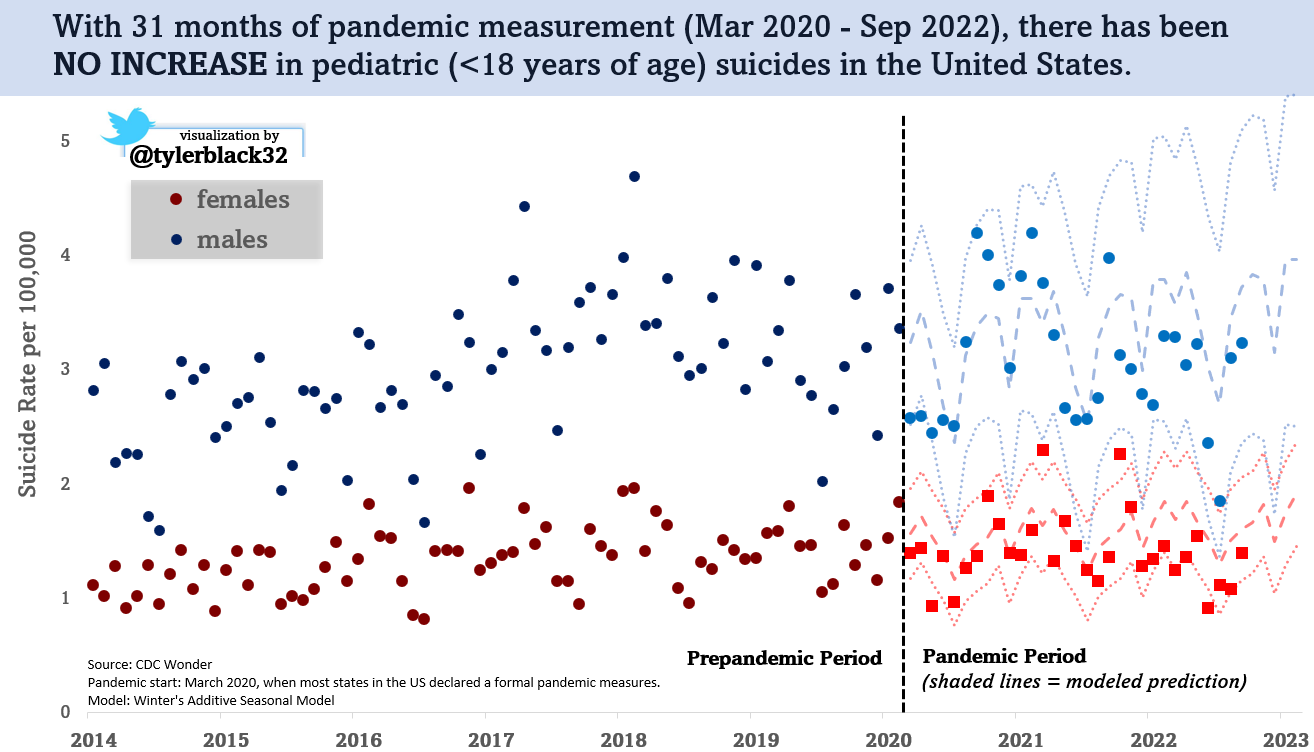
Furthermore, if we perform an extremely important check that visually eliminates seasonality from the analysis. By presenting linear trends for each month, we can get a clearer understanding of the data without the influence of seasonal fluctuations.
Upon examination, we can see that there are no months falling outside of the linear trends. In fact, if anything, the data indicates decreases in child suicides rather than increases.
The best “statistical test” of a time series is one that models for linear AND seasonal trends. In this case I’ve selected Winter’s Additive Seasonal Model, and when we do this we can clearly see the lack of major deviance from pre-pandemic trends. In fact, most of the observed months are below, not above, the predicted model.
The bottom line
The data I've analyzed provide robust evidence that for school-aged children, there has been no increase in pediatric suicides during the pandemic when compared to pre-pandemic trends. Furthermore, there is a strong possibility that we have actually witnessed a decrease in pediatric suicides during this time compared to prepandemic trends. This finding counters the concerns that the pandemic would lead to a significant increase in child suicides and highlights the resilience of children in these challenging times.
The implications
During the onset of the pandemic, many experts and organizations predicted a "tsunami" of suicides among children as a result of the crisis. This prediction was fueled by concerns over social isolation, economic instability, and uncertainty about the future. An article from the New York Times in January 2021 highlighted concerns from some one school district that the absence of in-person schooling could led higher suicide rates. Various news articles and headlines played into the moral panic surrounding these predictions, further spreading fear and anxiety about the potential consequences of the pandemic on children's suicide mortality. These types of headlines fueled concerns among parents, educators, and policymakers, leading many to believe that a significant rise in child suicides was inevitable.
The findings I’ve presented here demonstrate the importance of using data to inform our ideas, rather than succumbing to fears and moral panics (or worse, using our ideas to “shape” our data, as many in the research sphere have unfortunately done). As we've seen, the expected "tsunami" of pediatric suicides did not materialize. By relying on rigorous analysis and evidence-based research, we can make better decisions and develop more effective policies to support the mental health and well-being of children in times of crisis.





Hi, thanks for this. I wonder how you interpret the results recently published https://publications.aap.org/pediatrics/article/151/3/e2022058375/190657/Youth-Suicide-During-the-First-Year-of-the-COVID. Do you think it's because they are looking at a different range age?